Clinical Presentation
A 5-year-old, male Greyhound presented with rubbing at his nose and dysphagia. Neurological examination confirmed an abnormal, obtunded mental status with reduced facial sensation bilaterally. Otherwise considered healthy, the dog underwent a brain MRI using the Hallmarq 2nd generation 1.5T unit (see Fig 1 and 2).
Diagnostic Investigation
Fig 1 (A) T2W, (B) T1W pre-contrast and (C) T1W post-contrast transverse images – There is marked discontinuous contrast enhancement and thickening of the pachymeninges surrounding the cerebrocortex (purple arrow) and the trigeminal nerves are considered enlarged (red arrows) and markedly contrast-enhancing at the level of the entry of the foramen ovale.
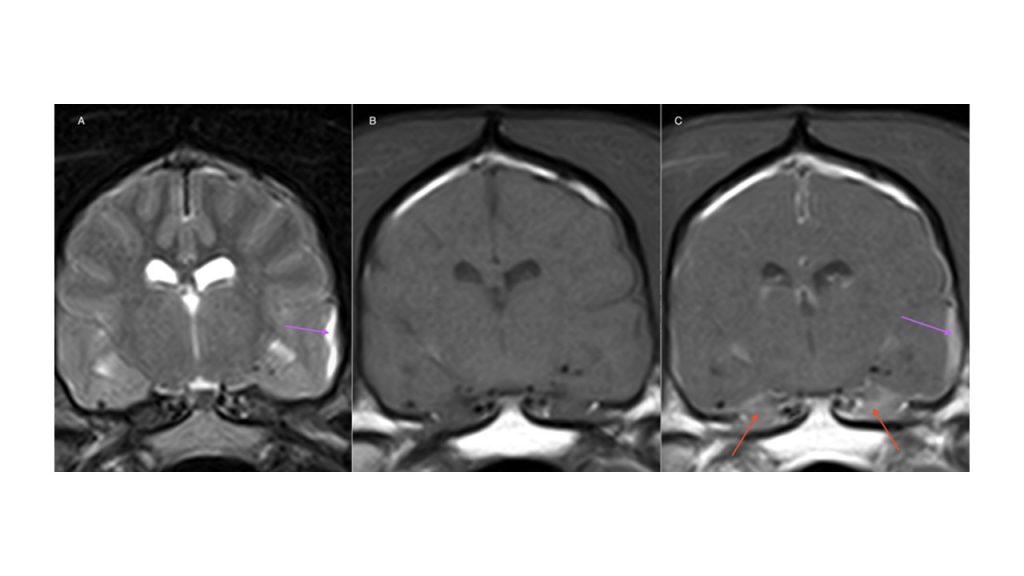
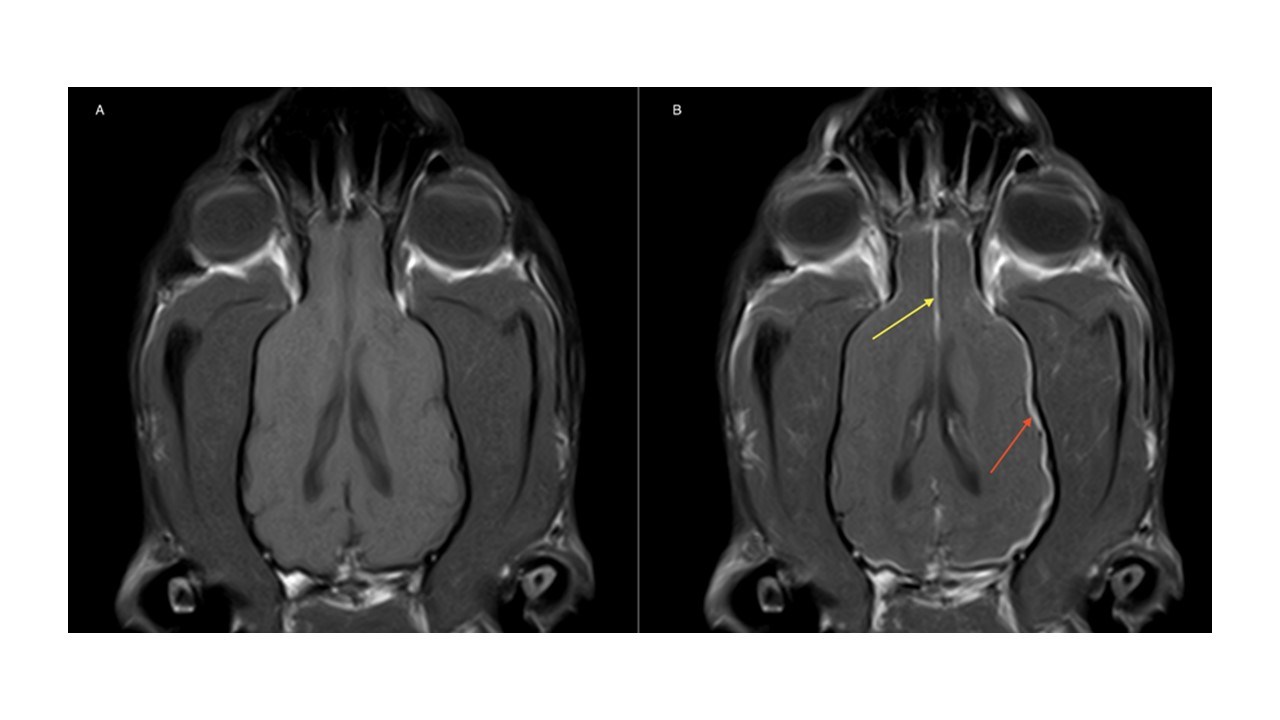
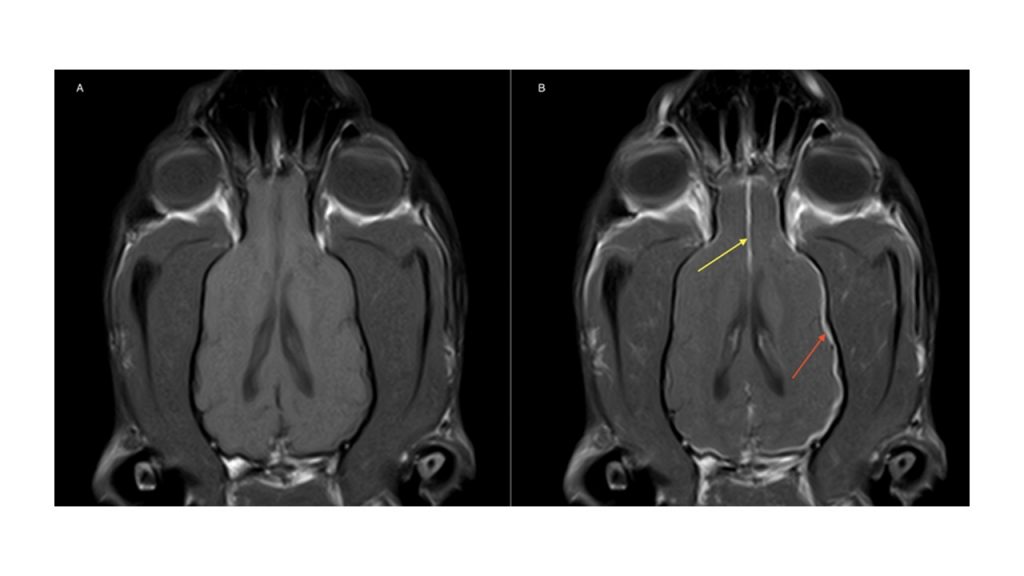
Fig 2 (A) T1W pre-contrast and (B) T1W post-contrast dorsal images – There is marked contrast enhancement and thickening of the pachymeninges surrounding the cerebrocortex (red arrow), more pronounced on the right side at the level of the occipital lobe, with partial involvement at the level of the falx cerebri (yellow arrow).
The Most Valuable MRI Sequence For This Case
The T1W post-contrast image reveals diffuse thickening and contrast uptake of the pachymeninges as the main finding here. This is strongly suggestive of hypertrophic meningitis, a condition Greyhounds appear predisposed to. Diffuse neoplastic processes affecting the meninges (meningeal carcinomatosis, lymphoma, granular cell tumor or histiocytic sarcoma) are considerations. However, all are less likely given the selective involvement of the pachymeninges without extension to the sulci, a characteristic which contrast administration is vital for the identification of and can be missed on other imaging sequences. Infectious diseases such as neospora and cryptococcus should also be ruled out with appropriate testing.
Disease Overview
Hypertrophic meningitis has previously been reported in dogs and suspected to be of immune-mediated origin. Most affected dogs are presented with multiple cranial nerve signs as a result of peripheral nerve involvement as they travel through the pachymeninges with the trigeminal nerve being the most documented cranial nerve to be affected, responsible for the loss of sensation in this case. MRI is essential for the presumptive diagnosis of this condition although it should be accompanied by CSF analysis which most often reveals a lymphocytic pleocytosis.
Histopathology has identified severe chronic, fibrotic, lymphoplasmacytic pachymeningitis resembling idiopathic hypertrophic pachymeningitis (IHP) in humans.
In humans, IHP is treated with glucocorticoids and other immunomodulating drugs such as azathioprine, cytosine arabinoside, methotrexate and cyclophosphamide. Treatment in veterinary medicine has been adapted from the treatment of CNS immune-mediated diseases and consists of the use of corticosteroids and cytosine arabinoside. Further studies are needed to evaluate other protocols and other immunomodulatory drugs (e.g., cyclosporine, procarbazine) in dogs. The prognosis can be guarded with recurrence being a feature of those initially successfully treated.
With thanks to Dr. Nick Shackleton RVN, and the Neurology Team at Dogwood Referrals for providing this case study.
References
Roynard P, Behr S, Barone G, Llabrés-Diaz F, Cherubini GB. Idiopathic hypertrophic pachymeningitis in six dogs: MRI, CSF and histological findings, treatment and outcome. J Small Anim Pract. 2012 Sep;53(9):543-8
Gonçalves R, De Decker S, Walmsley G, Butterfield S, Maddox TW. Inflammatory Disease Affecting the Central Nervous System in Dogs: A Retrospective Study in England (2010-2019). Front Vet Sci. 2022 Jan 27; 8:819945. doi: 10.3389/fvets.2021.819945.